Key Takeaways
- Colorado’s new budget law and executive order impose immediate Medicaid reimbursement cuts and reinstate prior authorization and claim review requirements.
- Providers should prepare for increased oversight from HCPF, including audits, recoupments, and stricter coverage determinations.
- Implementation begins September 1, 2025, leaving little time for providers to adjust operations and compliance processes.
On August 28, 2025, Governor Polis signed SB25B-001 – the primary bill resulting from the special session of the Colorado legislature. The session, convened on August 21, was called for the express purpose of addressing Colorado budget shortfalls arising from the federal spending legislation signed by President Trump earlier in July. The outcome of the federal legislation included a reduction of more than $1.2 billion in State revenue, and Colorado law requires a balanced budget.
SB25B-001, directs the Governor to balance the budget, and gives the Governor’s office the authority to “suspend or discontinue, in whole or in part, the functions or services of any department, board, bureau, or agency of the state government by Executive Order if the Governor determines there are not, or will not be, sufficient revenue available for expenditure during the fiscal year to carry on the functions of State government and to support its agencies and institutions.”1 The same day Governor Polis signed this bill, he released Executive Order D 2025-14, which outlines the various cost cutting measures the State of Colorado will take, effective as of September 1, 2025.
The news is particularly bleak for Colorado health care providers, as the specific cuts include:
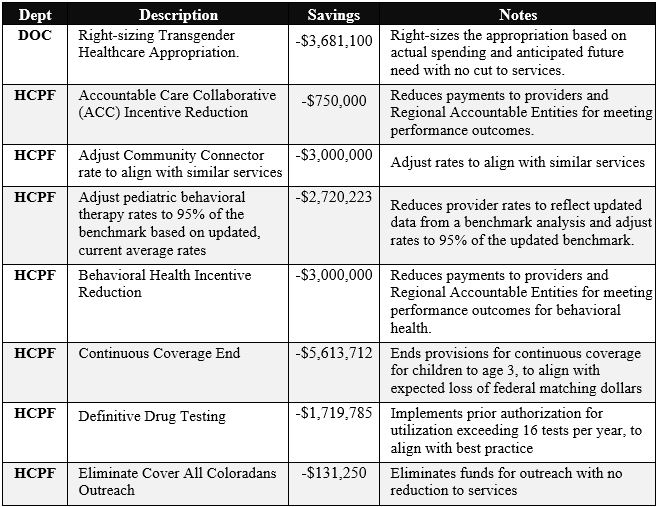
All told, Colorado health care providers bear $89,533,650 of the total budget adjustments. Behavioral health, developmental disability, and dental providers will see the most specific impacts, but all Medicaid providers will lose the benefit of the modest 1.6% increase in payments slated for this fiscal year.
Providers should also be aware that some of the projected savings come in the form of increased oversight from HCPF and other government agencies that could result in recoupment of funds already paid or in additional difficulty in obtaining coverage for services. For example, the Governor anticipates $7,000,000 in budget savings through the implementation of pre- and post-claim review of all pediatric autism therapy codes, another $1,700,000 in savings by implementing prior authorization requirements for definitive drug testing, and an additional $6,000,000 in savings from the reintroduction of prior authorization requirements for outpatient psychotherapy services.
With the September 1 effective date, providers across the board will see delays and cuts in payment almost immediately. Prior authorization and claim review components may take longer to implement, but providers should begin planning for compliance with these new requirements now.
Polsinelli is continuing to monitor program updates for more specific information, particularly implementation guidance and/or rulemaking from HCPF. We are also analyzing the impact of these cuts under federal and state law, particularly with respect to Colorado’s ability to maintain its obligations under its Medicaid State Plan and related waiver programs and its obligation to ensure parity between behavioral health and physical health benefits.
[1] Executive Order D2025-014 at 2. The full text of the Executive Order, along with the letter to the Joint Budget Committee detailing the specific cuts and cost saving measures, is available at https://leg.colorado.gov/sites/default/files/letter-08-28-25.pdf.





 />i
/>i
